For 66 percent of retirees, Social Security is their primary source of income.1 This may not have been a daunting financial undertaking for the federal government when the Social Security Act was originally signed into law in 1935. After all, life expectancy was just 63 years old at the time. Today, however, the population is living longer, much of the Baby Boomer generation is either in or nearing retirement, and current workers barely outnumber beneficiaries collecting Social Security. Therein lies a huge problem. Social Security was designed as a supplement to retirement income, not to be the primary source of income.
In the 1990s, the average retiree owned their home clear of any mortgage encumbrance, had a pension, and was receiving the supplemental Social Security benefit, as it was intended. However, the average client planning for retirement today is often in their third, fourth, or fifth job or company and still has a mortgage payment. Meanwhile, they are also attempting to save something for retirement while paying for their children’s college educations and often bearing the burden and expense of providing long term care for their parents. Unfortunately, managing these additional costs and burdens can result in a loss of income and cause physical, emotional, and financial suffering for the individual as well as their loved ones.
For many current clients, realizing these additional costs and caring for their aging parents has prompted them to consider their own future care. After all, the probability of needing long term care for individuals aged 65 and older is approximately 56 percent.2 That’s where long term care insurance comes in.
The History of Long Term Care Insurance and State Partnership in the United States
In 1935, President Franklin D. Roosevelt signed the Social Security Act (SSA) into law. Under the SSA, the Old Age Assistance program makes federal money available to the states to provide financial assistance to poor seniors. The law specifically prohibits making these payments to anyone living in public institutions, thus spawning the creation of the private nursing home industry.
In 1950, an amendment to the SSA required payments for medical care to be made directly to nursing homes rather than beneficiaries of care. Under the amendments, states were also required to license nursing homes to participate in the Old Age Assistance program.
In 1965, President Lyndon B. Johnson signed legislation enacting Medicare and Medicaid as amendments to the SSA. Medicare’s focus is on acute care only and does not provide for long term care. Medicaid allows for coverage of long term care in institutions but not in the home, creating a bias in favor of institutional care. Under this legislation, the federal and state governments became the largest payers for long term care, while nursing home utilization increased dramatically along with government expenditures.
In 1974, SSA amendments authorized federal grants to states for social services programs, including homemaker services, protective services, transportation, adult day care, training for employment, nutrition assistance, and health support. Final regulations for skilled nursing facilities were put into effect and enforcement of compliance with standards such as staffing levels, staff qualifications, fire safety, and delivery of services became a requirement for participation in Medicare and Medicaid. Several insurance companies launched the private long term care insurance industry with the intent of allowing individuals to purchase insurance policies that will pay for these necessary services and remove them from the public welfare system. Later policies expanded from coverage only for nursing homes to include home health care, assisted living facilities, memory care, and other variants often covered under alternate plans of care.
In 1992, four states (California, Connecticut, Indiana, and New York) implemented qualified state long term care partnership programs for their citizens. The following year, Congress enacted the Omnibus Budget Reconciliation Act, which prevented the expansion of these programs to the other forty-six states.
The Omnibus Budget Reconciliation Act of 1993 (or OBRA-93) was a federal law that was enacted by Congress and signed into law by President Bill Clinton on August 10, 1993. In terms of long term care insurance, this legislation established minimum standards to improve the quality of private insurance for long term care and tax incentives to encourage its purchase.
The Health Insurance Portability and Accountability Act of 1996 (HIPAA), Public Law 104-191, was enacted on August 21, 1996. HIPAA created tax qualified plans, deductibility of premiums paid, based on age. Individual and group plans that provide or pay the cost of medical care are covered entities. Health plans include health, dental, vision, and prescription drug insurers, health maintenance organizations (HMOs), Medicare, Medicaid, Medicare Choice and Medicare supplement insurers, and long term care insurers (excluding nursing home fixed-indemnity policies).
In 2005, Congress enacted the 2005 Deficit Reduction Act (DRA) which eliminated $40 billion of federal funding from state administered Medicaid programs but also provided the balance of the states the option of enacting their own partnership programs. The DRA provided federal funding to states to expand community-based care; authorized the Medicaid Money Follows the Person (MFP) Rebalancing demonstration program; allowed states to add an optional Medicaid state plan benefit for HCBS; and allowed states to offer self-direction of personal care services. It also lengthened the look-back period for transfers of assets for nursing home Medicaid applications from 36 to 60 months. In addition, it allowed for qualified state long term care partnerships, which encourage individuals to purchase long term care insurance while still allowing them to qualify for Medicaid if their care needs extend beyond the period covered by their insurance policy.
The Government Takes Action
In 2023, the largest line item in most state budgets is Medicaid. Even with funding from the federal government, states struggle with this particular expense because of the ever-growing need for long term care required by its citizens. If the Baby Boomers as a cohort require the level of long term care that is anticipated and if they have not purchased private long term care insurance, this comprehensive expense will break the Medicaid bank.
Congress has made a token gesture at preventing this disaster by passing legislation that encourages the purchase of private long term care insurance, tax qualifying these plans with accompanying deductibility of premiums, as well as the advent, and eventual expansion, of the partnership programs.
Currently, the states themselves are finally taking action to prevent this tsunami from breaking their respective banks. In 2021, Washington State launched the Washington Cares Fund,3 which created a 0.58 percent tax on all W-2 employees aged 18 years and older. This prompted the public to purchase some 470,000 traditional and non-traditional long term care policies in order to opt out of this tax.4 Whereas Washington State generated only about three percent of national LTCI sales in 2020, this surge in sales ultimately accounted for 60 percent of national sales in 2021.5 To date, there are 10 other states in various stages of considering a like program for their own citizens.
Qualifying for Medicaid
Despite the WA Cares Fund and other states considering similar programs, the reality is Medicaid continues to be an essential resource for seniors who require long term care. However, in order to qualify for Medicaid assistance, an applicant must have assets and income below specific levels established by each state. Applicants in most states are limited to $2,000 in countable assets in addition to exempt assets, such as a marital home, one vehicle, and other personal effects. Applicants typically must spend down any assets that exceed these limits to meet this threshold and financially qualify for Medicaid.
Medicaid also has a standard lookback period of five years in most states. The two most notable exceptions to the five-year lookback period are California, which limits it to 30 months, and New York, which is in the process of fielding a similar provision. During this period, the applicant may be penalized based on any divestments made by them or their spouse. If Medicaid determines the lookback period has been violated, the applicant will be penalized based on the dollar amount they have transferred to others. This penalty is calculated using a state-specific penalty divisor, which is determined based on the average monthly cost of a nursing home in a specific state.
Example: Calculating the Medicaid Penalty Period
John applies for long term care Medicaid on January 2, 2023. Within the lookback period of 60 months, Jim sold his cottage to his son for $20,000, much lower than the fair market value of $120,000, and gifted his granddaughter $15,000 for college. John has disqualifying transfers in the amount of $115,000 ($100,000 for the house + $15,000 gifted). In John’s state, the penalty divisor is $8,500/month. For every $8,500 gifted or sold under fair market value, John will be penalized with a month of Medicaid ineligibility. Therefore, John will be penalized with 13.5 months of ineligibility ($115,000 ÷ $8,500 = 13.5 months), during which time John must pay privately for his care before Medicaid begins.
How the LTCI Policy Works with the Medicaid Program
State partnership-qualified long term care insurance policies essentially form a partnership, or better, a collaboration, between private insurance companies and the public government. Partnership policies exist for the expressed purpose of encouraging the purchase of these policies to help cover the costs of long term care while diminishing the burgeoning burden on the states to pay the high costs associated with long term care, which continues to be the single largest line item in each state’s Medicaid budget.
State partnership plans offer policyholders dollar-for-dollar protection and can serve as excellent estate planning and asset preservation tools. Owners of partnership qualified LTCI plans can protect some, or in some cases all, of their estates, depending on the depth and breadth of the plan and the size of the estate as well as the length and degree of required care.
In the event the policyholder exhausts their LTCI benefits and must continue with care under Medicaid, the assets that were protected by a partnership qualified LTCI policy are also safe from Medicaid’s mandated asset recovery program, further ensuring these assets remain as inheritance for family after the passing of a Medicaid recipient. This also allows Medicaid recipients to, in essence, retain assets above and beyond the limits set forth by Medicaid.
To date, nearly all states have their own version of partnership. States that do not currently have partnership are Alaska, Hawaii, Mississippi, and the District of Columbia.
The huge advantage of the asset protection afforded by a partnership qualified LTCI policy is that an individual, or couple if purchasing a shared plan, can protect additional funds, dollar-for-dollar, based on the amount of coverage paid out by the plan, and subsequently qualify for coverage. For most people, the single largest asset that they possess is the family home. With a qualified partnership LTCI policy, a Medicaid recipient can declare their home as a “protected” asset, thus protecting it from the mandated Medicaid estate recovery program. This allows the home to remain with the family as inheritance.
Example: Partnership Qualified LTCI
Scott has always been a planner, so when he met with his advisor he decided to purchase a partnership qualified LTCI policy. He faithfully paid the premiums over the years, and because of the inflation rider partnership required, the policy’s pool of benefits grew. Eventually, Scott’s family and doctor determined that Scott’s declining health and his inability to perform two of the six activities of daily living warranted filing a claim with his LTCI carrier. Ultimately, over the course of three years, he received reimbursed benefits totaling $300,000 before the policy pool was exhausted. Still very much alive and in need of care, Scott’s family assisted him in applying for Medicaid. At the time of application, Scott’s house was valued at $225,000, and he had modest cash on hand in a checking account of about $85,000. Because of his partnership qualified LTCI policy, Scott was eligible to retain $300,000 (his home and cash assets) in addition to his standard allowance of $2,000 while still qualifying for Medicaid.
Requirements for a Policy to Be Eligible for a State Partnership Program
A long term care partnership policy provides the added benefits of offering those who own them a way to protect their assets, dollar-for-dollar, in the amount of policy benefits paid out on their behalf in the event they ever need to apply for long term care benefits under a particular state’s Medicaid program. Additionally, a long term care partnership policy has beneficial tax treatment and requires inflation protection features that protect younger purchasers from increases in expenses caused by inflation.
For most people, the benefits of a partnership policy are likely to cover all the care they will ever need. However, because of the unique asset protection feature, they won’t have to impoverish themselves if they run out of benefit coverage and still need care. The individual plans must conform with federal guidelines in terms of tax qualification, benefit triggers, and other defined conditions. Partnership plans are portable and can be utilized in any state, provided both states have partnership programs and mutual reciprocity agreements.
Partnership plans accentuate the very reasons people have purchased this form of insurance for nearly fifty years since they prevent them from becoming burdens on their family. Additionally, long term care insurance assists in maintaining their independence, prevents the dissipation of assets, and preserves their personal dignity. It also prevents them from becoming dependent upon the government for welfare assisted services.
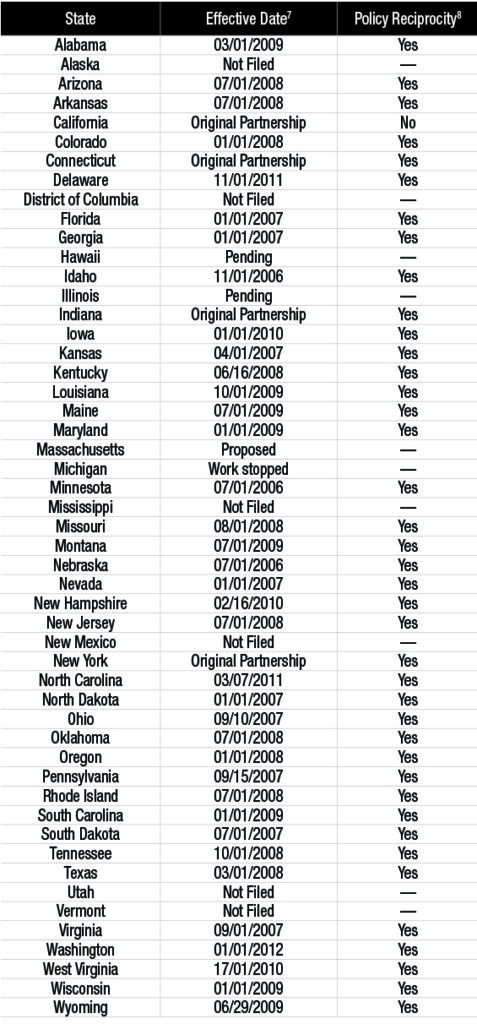
The Table To The Right Shows States That Have Approved Long Term Care Partnership Insurance.6
Alternative Policy Design Options Your Clients May Want to Consider
Traditional long term care insurance saw its high-water mark in 2002 with over $1.024 billion in policy sales.9 Since that year, sales for the traditional product offerings have dropped (with only an occasional bump in sales that reversed this trend) with more and more consumers and producers flocking to hybrid/combination/asset-based products that usually consist of life insurance with a long term care rider or an annuity with a long term care rider.
These policies have great appeal to people who fear they will not use the policy and essentially waste these premium dollars. For them, the “Live Die Quit” mantra may be presented because if they do live and require long term care, the policy will have available benefits; if they do not use the long term care aspect of the policy, they will eventually die and their beneficiaries can avail themselves of the death benefit; or, if they change their mind down the road, they can recover their invested principal.
Conclusion
With the advent of new pharmaceuticals, advancements in the practice of medicine, and changes to lifestyle and eating habits, as a society we are lingering longer. When Theodore Roosevelt was President of the United States at the beginning of the twentieth century, life expectancy was only 47 years of age. Today, it is more than 81. While the U.S. is faring better than many other countries, our demographics reveal a population that is aging in place with diminished available savings and a growing need for long term care.
As more Americans require long term care, Medicaid continues to be the largest payer of these costs. Therefore, the elderly will only continue to apply for benefits in order to meet long term care needs at the end of their lives. Long term care insurance, particularly those plans that are partnership-qualified, will make a huge difference in the lives of individuals, their families, and on society as a whole.
Because of the growing need for long-term care insurance, the wide array of available products makes it a must-have for all portfolios. State partnership has proven to be a wonderful addition to the formula, as people can safeguard assets, establish and protect financial legacies, and still enjoy the much-needed care they will likely need at the end of their life.
Private long term care insurance is an economical way for individuals and couples to protect their savings and provide themselves with a variety of options regarding their long term care. It allows them to pay for these services without exhausting their retirement assets or family savings. It also affords them choice as to where they wish to receive these services. A partnership-qualified plan further allows them to safeguard, on a dollar-for-dollar basis, a portion of their estate equal to the amount of money disbursed by the issuing carrier on a reimbursement basis.
Reference:
- A Precarious Existence: How Today’s Retirees Are Financially Faring in Retirement, TransAmerica Center for Retirement Studies, December 2018, https://www.transamericacenter.org/docs/default-source/retirees-survey/tcrs2018_sr_retirees_survey_financially_faring.pdf.
- Projections of Risk of Needing Long-Term Services and Supports at Ages 65 and Older, U.S. Department of Health and Human Services, January 2021, https://aspe.hhs.gov/sites/default/files/private/pdf/265136/LTSSRisk.pdf.
- WA Cares Fund, 2021, https://wacaresfund.wa.gov/about-the-wa-cares-fund/.
- Washington State Retools First-in-the-Nation Long-Term Care Benefit, Kaiser Health News, April 2022, https://khn.org/news/article/washington-state-retools-first-in-the-nation-long-term-care-benefit/.
- 2022 Milliman Long Term Care Insurance Survey, Broker World Magazine, July 2022, https://brokerworldmag.com/2022-milliman-long-term-care-insurance-survey/.
- American Association for Long-Term Care Insurance, March 2014, https://www.aaltci.org/long-term-care-insurance/learning-center/long-term-care-insurance-partnership-plans.php.
- The Effective Date is the date the U.S. Department of Health & Human Services approved the state plan amendment. Original Partnership indicates one of the four original partnership states.
- Policy Reciprocity indicates whether the state will honor partnership policies from other DRA partnership states when it comes to allowing asset disregard when filing for Medicaid. All DRA states plus New York, Indiana, and Connecticut have reciprocity. California does not.
- LTC Insurance and Medicare Supplement Executive Summary, Annual 2002, LIMRA International.




