The 2019 Milliman Long Term Care Insurance Survey is the 21st consecutive annual review of stand-alone long-term care insurance (LTCI) published by Broker World magazine. It analyzes the marketplace, reports sales distributions, and describes available products including group insurance.
More analysis of worksite sales will appear in the August issue of Broker World magazine.
Unless otherwise indicated, references are solely to U.S. stand-alone LTCI sales, excluding exercised future purchase options (FPOs) or other changes to existing coverage. “Stand-alone” refers to LTCI policies that do not include death benefits (other than returning premiums upon death or waiving a surviving spouse’s premiums) or annuity or disability income benefits. Where referenced, “combo” policies provide LTCI combined with life insurance or annuity coverage.
Highlights from This Year’s Survey
Participants
Eleven carriers participated broadly in this survey. Four others provided sales information so we could report more accurate aggregate industry individual and multi-life sales. From these submissions, we estimated total industry production.
We estimate our statistical distributions reflect up to 90 percent of total industry sales and about 65 percent of worksite sales.
State Farm discontinued stand-alone LTCI sales in May 2018, hence is no longer included in the Product Exhibit.
Although not displaying products, Northwestern LTC and State Farm provided background statistical information. Auto-Owners, LifeSecure, Transamerica and United Security Life contributed total and worksite sales (new premium and lives insured) but did not provide broad statistical information.
Sales Summary
- The 15 carriers reported sales of 56,288 policies and certificates (“policies” henceforth) with new annualized premium of $171,537,644 (including exercised FPOs) in 2018, compared to 2017 restated sales of 64,800 policies ($181,506,770 of new annualized premium), a 13.1 percent drop in the number of policies and a 5.5 percent drop in the amount of new annualized premium. As noted in the Market Perspective section, sales of policies combining LTCI with other risks continue to increase.
- Five of the top 10 insurers sold more new premium than in 2017, but only three sold more new policies. This difference emerges because elected FPOs add on-going premium but not new policies.
- With FPO elections included in new premium, Northwestern garnered the number one spot in new sales. Mutual of Omaha was a strong second and had a large lead in annualized premium from new policies sold. Together, they combined for 57 percent of new premium including FPOs and 52 percent of new premium excluding FPOs.
- For the fourth straight year (and fourth time ever), our participants’ number of inforce policies dropped, this time by 1.1 percent, after 5.1 percent (2017), 0.3 percent (2016) and 0.2 percent (2015) drops previously.
- Nonetheless, year-end inforce premium per policy continues to increase (3.0 percent in 2018) to $2,169. Inforce premium increases from sales, price increases, and benefit increases (including FPOs), and reduces from lapses, reductions in coverage, deaths, and shifts to paid-up status for various reasons.
- Participants’ individual claims rose 5.9 percent. Overall, the stand-alone LTCI industry incurred $11.0 billion in claims in 2017 based on companies’ statutory annual filings, raising total incurred claims from 1991 through 2017 to $129.9 billion. (Note: 2017 was the most recent year available when this article was written.) Most of these claims were incurred by insurers that no longer sell LTCI. The reported 2017 incurred claims is similar to the $11.1 billion of incurred claims reported in 2016. Combo LTC claims are in their infancy and amounted to $5.9 million. The claim figures are even more startling considering that only a small percentage of the 7 million covered individuals were on claim at the end of 2017.
- The average processing time in the industry was eight percent faster in 2018 than in 2017. Nonetheless, active policies resulted from only 58.8 percent of applications, even lower than 2017’s record low of 59.0 percent. Financial advisors often are reluctant to risk a bad experience by recommending that clients apply for LTCI. As noted in the Market Perspective section, the industry may be able to improve placement rates in a variety of ways.
About the Survey
This article is arranged in the following sections:
- Highlights provides a high-level view of results.
- Market Perspective provides insights into the LTCI market.
- Claims presents industry-level claims data.
- Sales Statistical Analysis presents industry-level sales distributions reflecting data from 11 insurers
- Partnership Programs discusses the impact of the state partnerships for LTCI.
- Product Exhibit (click here for PDF) shows, for nine insurers: financial ratings, LTCI sales and inforce, and product details.
Click here to view the following additional information available only online.
- Product Details, a row-by-row definition of the product exhibit entries, with a little commentary.
- Premium Exhibit shows lifetime annual premiums for each insurer’s most common underwriting class, for issue ages 40, 50, 60, and 70 for single females, single males, and heterosexual couples (assuming both buy at the same age), based on $100 per day (or closest equivalent weekly or monthly) benefit, 90-day facility and most common home care elimination period, three-year and five-year benefit periods or $100,000 and $200,000 maximum lifetime buckets, with and without Shared Care and with flat benefits or automatic three percent or five percent annual compound benefit increases for life. Worksite premiums do not reflect any worksite-specific discount, though some carriers offer this.
- Premium Adjustments (from our published prices) by underwriting class for each participant.
- Distribution by underwriting class for each participant.
- State-by-state results: percentage of sales by state, average premium by state and percentage of policies qualifying for Partnership by state.
Market Perspective (more detail in subsequent parts of the article)
- The stability of current prices bears no resemblance to the past instability because today’s prices reflect much more conservative assumptions based on far more credible data and low investment yields. Unfortunately, many financial advisors presume that new policies will face steep price increases. It is likely to take a long time before the market becomes comfortable that prices are stable.
- Combo products have increased market share because: i) their other benefits mean that regardless of whether the policyholder has a long term care claim, they will receive benefits, ii) they often have guaranteed premiums and benefits, and iii) they now offer alternatives besides single premium.
According to LIMRA, combo life policies (LTCI combined with life insurance) represented 16 percent of new 2017 annualized life insurance premium (25 percent and $4.1 billion, if you include 100 percent of single premium sales). Fourteen percent of the 260,000 combo policies included LTCI benefits after the death benefit had been fully advanced (“extension of benefits; EOB”). Of the 86 percent in which LTCI benefits could not exceed the death benefit, nearly six in 10 (57 percent) used “chronically ill” provision that is not allowed to be called “long term care insurance”, rather than a §7702 LTCI provision.
Looking at the total LTCI market, stand-alone policies accounted for 20.0 percent of the 2017 policies sold, policies with extensions of benefits (EOB) accounted for 11.2 percent and policies with accelerated death benefits but no EOB accounted for 68.8 percent.
- As anticipated in last year’s report, a new entrant offers unisex LTCI pricing for the worksite market, another carrier re-entered the worksite market and a third carrier is test-marketing a worksite product for possible release. In addition, more combo products are being proposed in the worksite market. For businesses with employees residing in multiple jurisdictions, consistent product availability can be a challenge. Worksite LTCI is more attractive to employers when packaged with solutions for employees who are caregivers for their elders.
- As noted earlier, fewer than 59 percent of applications have resulted in issued policies in the past two years. The low placement rate makes financial advisors hesitant to recommend that clients consider LTCI. The industry may be able to improve placement rates in a variety of ways.
- E-applications make the process faster, secure better health information (some applications may then not be submitted) and avoid long delays on apps that are “not in good order” when submitted. In our 2018 survey article, we reported that eApps were 71 percent more likely to be in good order and were less likely to be declined. It would be helpful if brokerage general agents could populate an eApp with quote information, then forward that partial eApp to the broker for completion.
- Better pre-qualification of prospects’ health will guide applications to an insurer most likely to accept the applicant. As noted above, eApps help. If advisors are reluctant to discuss health issues with their clients, some general agencies interview the client on behalf of the advisor or provide a link to a website where the client can answer health questions. Data quantifying the positive impact of thorough pre-qualification would be helpful.
- Higher placement rates result when cash is required with the application (CWA). This year, we asked insurers for data regarding placement (excluding worksite business) based on whether cash was required with the application. Carriers who accept applications with or without cash reported a combined placement rate of 58.1 percent with cash and 54.0 percent without cash. Insurers which reported only CWA data placed 60.4 percent of their cases. Insurers which reported only data without CWA placed 55.0 percent.
- Faster processing may help. However, as noted earlier, the average processing time was 10 percent faster in 2018 than in 2017, yet the placement rate still dropped 0.2 percent. Maybe it would have dropped more without the faster processing.
- Better messaging regarding the value of LTCI and about the value of buying now (rather than in the future) would improve the placement rate (as well as increase the number of applications).
- Insurers may be able to educate their distribution system more effectively, such as with drill-down questions in on-line underwriting guides.
- Three participants have never increased premiums on policies issued under “rate stabilization” laws. Three insurers reported that their highest cumulative increase on such policies has been about 40 percent and two had increased prices 100 percent or more. Two carriers did not indicate their maximum increase, one of which we believe was in the lower end and one in the higher end.
All the insurers allow clients to reduce the maximum daily/monthly benefit (typically not below the original minimum) with a proportionate reduction in future premium. All allow clients to move to a shorter originally-available benefit period with premiums the same as they would currently be had they purchased that benefit period originally. Eighty percent of the insurers allow clients to select a longer elimination period, with premiums the same as they would currently be had they purchased that longer elimination period initially. Some insurers may not offer this option because they do not have longer elimination periods available.
If a client drops a compound benefit increase rider, most insurers freeze the current benefit and charge the premium that the client would be paying today had the client purchased the current amount originally with no compound benefit increases. One insurer takes a more consumerist approach, freezing the benefit and reducing the current premium by the cost of the benefit increase rider. Some policyholders may face reversion to the original maximum daily or monthly benefit.
One insurer explained that the above approaches for dropping a compound benefit increase rider result in higher future premiums as a result of sacrificing future benefit increases if the maximum daily/monthly benefit has increased beyond the additional percentage cost for the compound benefit increase rider. Therefore, that insurer suggests that clients reduce the daily/monthly maximum benefit and retain compounding.
- Our projected amount of issued protection on new policies increased significantly in 2018 because an insurer with negative-election FPOs (negative-election FPOs activate automatically unless the client rejects them, as opposed to positive-election FPOs which activate only if the client makes a request) submitted FPO election rate data this year but not last year. For the average 57-year-old purchaser in 2018, we project a maximum benefit in 2041 of $313/day, equivalent to an average 3.0 percent compounded benefit increase. Had he/she purchased last year’s average policy at age 56, he/she would have had $279/day by age 80, equivalent to 2.3 percent compounding. Without the change in insurers providing FPO data, the age 80 maximum daily benefit would have dropped from $279 to $276. Purchasers may be disappointed if the purchasing power of their LTCI policies deteriorates over time.
- Claimants rarely challenge insurer claim adjudications. Since 2009 (varies by jurisdiction), if an insurer concludes that a claimant is not chronically ill, the insurer must inform the claimant of his/her right to appeal the decision to independent third-party review (IR). The IR determination is binding on insurers. As shown in our Product Exhibit, most participants have extended IR beyond statutory requirements, most commonly to policies issued prior to the effective date of IR. At least four participating insurers report never having a request for IR. Four other insurers have reported a total of 72 IR requests resulting in the insurers’ denials being upheld more than 90 percent of the time. This data is consistent with the experience of LTCI Independent Eligibility Review Specialists, LLC. Steve LaPierre, president of that firm, indicated that they have performed approximately 125 IRs and have upheld the insurer more than 90 percent of the time. The existence of IR, the insurers’ voluntary expansion of IR and the insurer success rate when appeals occur help justify confidence in claim decisions.
- Only four participants offer coverage in all U.S. jurisdictions and no worksite insurer does so. Insurers are reluctant to sell in jurisdictions which are slow to approve new products, restrict rate increases, or have unfavorable legislation or regulations.
- Seven of our 11 participants use reinsurers and seven use third party administrators (TPAs). The reinsurers are Reinsurance Group of America, LifeCare, Manufacturers, Swiss Re and Union Fidelity. The TPAs are Long-Term Care Group, Life Plans, LifeCare Assurance, and CHCS. Other reinsurers and TPAs support insurers not in our survey. In some cases, affiliated companies provide reinsurance or guarantees.
- A significantly-changed LTCI Shopper’s Guide was recently adopted by the NAIC. We’re interested in readers’ reviews of the new Guide and comments as to how much it is used to educate consumers. (Please email comments to claude.thau@gmail.com.)
Claims
- Ten participants reported 2018 claims. The consistency of the data is improving, but some companies were not able to respond to some questions or could not respond in a way that justified including their data for some questions.
- For the ten insurers which reported individual claims for both 2018 and 2017, claim dollars rose 5.9 percent, despite a 1.1 percent decrease in inforce policies.
- The LTCI industry has had a much bigger impact than indicated above, because a lot of claims are paid by insurers that no longer sell LTCI.
LTCI claims paid by insurers no longer selling LTCI likely differ significantly from data reported below as their claimants are more likely to have facility-only coverage, be older, etc.
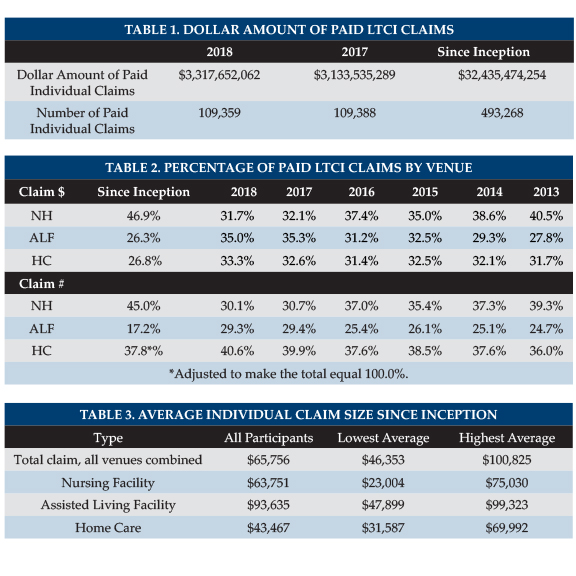
Table 1 shows the total dollar and number of individual LTCI claims paid by those carriers which provided information to use.
Table 2 shows the distribution of those claims by venue. In the distribution based on number of claims, a person who received care in more than one venue is counted once for each venue, but not double-counted in the total line. Individual claims in general continue to shift away from nursing homes. We expect on-going shift away from nursing homes due to consumer preferences and more claims coming from comprehensive policies.
Six of eight carriers that submitted their number of open claims at year-end reported a pending number of claims between 57 percent and 84 percent of the number of claims paid during the year.
Table 3 shows average size individual claims since inception, all of which rose compared to 2017. Because claimants can submit claims from more than one type of venue, the average total claim generally exceeds the average claim paid for any particular venue. Nonetheless, individual ALF claims are consistently high, probably because:
a) ALF claims appear to last long compared with other venues.
b) Nursing home costs are most likely to exceed the policy daily/monthly maximum. Hence the maximum daily benefit negates part of the additional daily cost of nursing homes.
c) People who maximize the use of their maximum monthly benefits can spend as much on an ALF as on a nursing home.
d) Although some surveys report that ALFs cost about half as much as nursing homes on average, ALFs often charge more for a memory unit or more substantial care for levels of assistance that align more closely with nursing home care. And upscale ALFs seem to cost a higher percentage of upscale nursing home costs than the average ALF/nursing home ratio.
Some people may have expected ALF claims to be less expensive than nursing home claims because ALFs cost less per month. But that has not been the case. Some observers applaud insurers which have extended ALF coverage to policies which originally did not include ALF coverage, even though such action has contributed to rate increases on in force policies.
The following factors cause our average claim sizes to be understated.
- Roughly 1/8 of the inception-to-date individual claims are still open. Our data does not include reserve estimates for future payments on open claims.
- People who recover, then claim again, are counted as multiple insureds rather than adding their various claims together.
The range of average claim results by insurer (see Table 3) is startling. What can contribute to such differences?
- Different markets (by affluence; worksite vs. individual; by geography; etc.).
- Different lengths of time in the business. A newer issuer may have a higher percentage of open claims bringing down the average.
- Percentage of policies sold to women or with compound benefit increases, monthly home care determination, or 50 percent home care benefits or reduced benefits for ALFs.
- Distribution by elimination period. Zero-day EP policies might result in a lot of small claims. Ironically 180-day or longer EPs could also result in relatively small claims.
- Perhaps erroneous reporting. In some of our calculations we have eliminated some submitted data because it seemed very unlikely to be accurate.
Average claim data understates the value of buying LTCI because the many small claims drive down the average claim. LTCI can provide significant financial return for people who need care one year or longer. The primary purpose of insurance is to protect against adverse results, so the amount of protection, as well as average claim, is important.
Six insurers were able to provide data regarding their current monthly exposure. The average current monthly maximum nursing home benefit per inforce claimant ranged from $4,575 to $8,182.
The six insurers’ total monthly exposure (including non-claimants) exceeds $5.5 billion, more than thirty times their corresponding monthly premium income. Recognizing that claims can continue up to the full benefit period, these insurers’ potential claim exposure is about 120 times their monthly premium income.
Nursing home (NH) claims are more likely to use the policy’s maximum daily/monthly benefit than ALF claims, because ALF costs are generally lower and because policies sometimes have lower maximums for ALFs. ALF claims correspondingly are more likely to use the policy maximum than are adult day care and home care claims.
Statistical Analysis
Eleven insurers contributed significant background data, but some were unable to contribute data in some areas. Four other insurers (Auto-Owners, LifeSecure, Transamerica and United Security) contributed their number of policies sold and new annualized premium, distinguishing worksite from other sales.
Sales characteristics vary significantly among insurers. Year-to-year variations in policy feature distributions may reflect changes in participants, participant practices and designs, participant or worksite market shares and industry trends.
Market Share
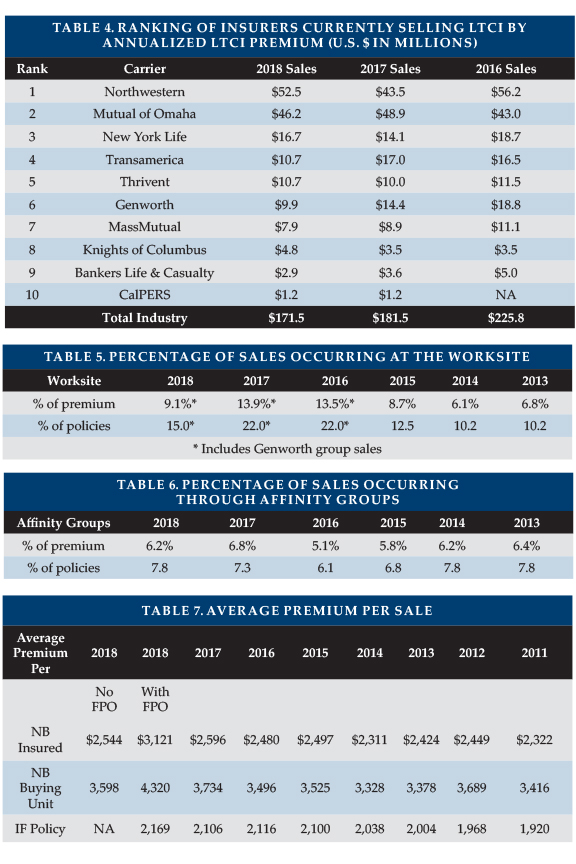
Table 4 lists the top 10 participants in 2018 new premium, among those still offering LTCI. Because we include FPO elections, Northwestern surpassed Mutual of Omaha. Without FPOs, Mutual of Omaha would have been number one. Together, they produced 57 percent of annualized new premium in 2018 and 52 percent of annualized premium on new policies. They are followed by five insurers with four percent to 10 percent market share each.
Worksite Market Share
Worksite business produced 15.0 percent of new insureds (see Table 5), but only 9.1 percent of new premium (including FPOs) because of its younger issue age distribution and less robust coverage. Worksite sales consist of three different markets:
- Voluntary group coverage generally is less robust than individual coverage.
- Core/Buy-Up programs have particularly young age distributions and modest coverage because a lot of people do not buy-up and are least likely to insure spouses.
- Executive carve-out programs generally provide the most robust coverage. One- or two-couple executive carve-out sales may not qualify for a multi-life discount with some insurers, hence may not be labeled as worksite sales in submissions to our survey.
The amount of worksite sales reported and its distribution among the three sub-markets significantly impact product feature sales distributions. Although Table 5 reflects the full market, this year’s policy feature distributions underweight the voluntary and core/buy-up markets because carriers in those markets shared less policy feature distribution data. More information about worksite sales will appear in the August issue of Broker World magazine.
Affinity Market Share
The affinity sales percentage is based on the participants who provide significant statistical data. Their reported affinity sales produced 7.8 percent of their new insureds (see Table 6), but only 6.2 percent of premium. Only about 20 percent of the lower affinity average premium is attributable to the affinity discount. The balance may be due to younger issue age or less robust coverage.
Characteristics of Policies Sold
Average Premium
As noted last year, our inclusion of FPOs as new business premium overstated the average premium per new insured and buying unit (Table 7) increasingly over time. More precise queries this year allow us to quantify the impact. The average premium per new life ($2,544) is 18 percent less than we would have quoted including FPOs in the numerator. Three insurers reported average premiums for new insureds below $1,700, while five insurers were over $2,800. The average premium per new buying unit (counts a couple only once) was $3,598.
The lowest average new premium (including FPOs) was in Puerto Rico ($1,960), followed by Kansas ($2,448), while the highest was in New York ($4,243), followed by Connecticut ($3,886).
Due to rate increases, FPO elections and termination of older policies, the average inforce premium jumped to $2,168, 3.0 percent more than our restated 2017 figure.
Issue Age
Table 8 summarizes the distribution of sales by issue age band based on insured count. The average issue age was 56.6. The higher average issue ages of the past two years are partly caused by not having issue age distribution for some worksite business. Furthermore, two participants have a minimum issue age of 40, one won’t issue below 30, and two won’t issue below 25.
Benefit Period
Table 9 summarizes the distribution of sales by benefit period. The average notional benefit period slightly increased from 3.73 to 3.74. Because of Shared Care benefits, total coverage was higher than the 3.74 average suggests. For the first time, a single benefit period (3-year) accounted for half the sales.
Monthly Benefit
Table 10 shows that monthly determination applied to 77.8 percent of 2018 policies. With monthly determination, low-expense days leave more benefits to cover high-expense days. When it is offered as an option, we conclude that more than 50 percent of buyers opt for monthly determination. Measuring election rates for optional monthly determination can be challenging due to influences such as insurers switching products during the course of a year and state variations.
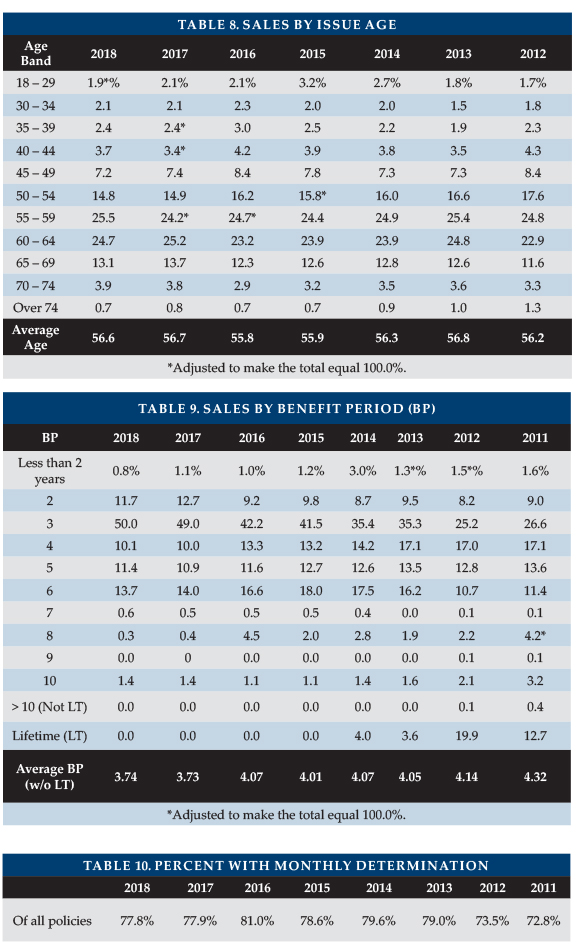
Table 11 summarizes the distribution of sales by maximum monthly benefit at issue. Sales were more clustered between $4,500 and $5,999/month than in any year since 2011. The average initial maximum monthly benefit was $4,763, almost exactly the average of 2015-2017.
Benefit Increase Features
Table 12 summarizes the distribution of sales by benefit increase feature. “Other compound” has grown a lot in the past two years; most involve three percent compounding.
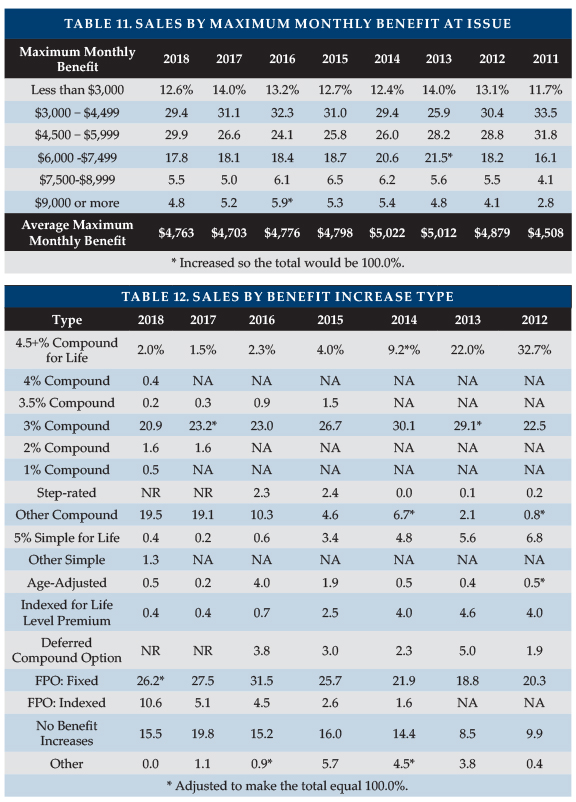
The increase in “FPO: Indexed” and the decrease in policies having “no benefit increases” were caused by a reclassification of an insurer’s sales. The insurer guarantees to offer FPOs of indeterminate amount, but the insurer bases its decision on interest rates.
Five percent compounded for life, which represented 56 percent of sales in 2003 and more than 47.5 percent of sales each year from 2006 to 2008, now accounts for only two percent of sales. Simple five percent increases for life were 19 percent of 2003 sales but are now only 0.4 percent of sales.
“Indexed Level Premium” policies are priced to have a level premium, but the benefit increase is tied to an index such as the consumer price index (CPI).
We project the age 80 maximum daily benefit by increasing the average daily benefit purchased from the average issue age to age 80, according to the distribution of benefit increase features, using current future purchase option (FPO) election rates, a five percent/year offer for fixed FPOs and assuming a long-term three percent CPI. The maximum benefit at age 80 (in 2041) for our 2018 average 57-year-old purchaser projects to $313/day (equivalent to 3.0 percent compounding). Had our average buyer bought an average 2017 policy a year ago at age 56, her/his age 80 benefit would be $279/day (equivalent to 2.3 percent compounding). This healthy increase in age 80 maximum benefit (from $279/day to $313/day) is attributable to the inclusion of an additional carrier in the data (see Table 14 discussion). Without that insurer, the projected age 80 maximum daily benefit would have dropped from $279 to $276. Most policyholders seem likely to experience eroding purchasing power over time if cost of care trends exceed three percent.
Eight insurers reported new premium from FPO elections; the percentage of their new premium that came from FPOs ranged from two percent to 43 percent.
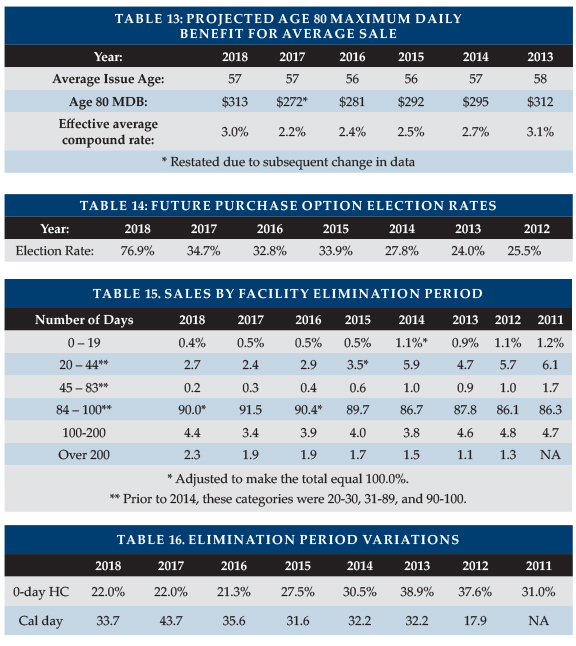
Seven insurers provided the number of available FPOs in 2018 and the number exercised. Six of those insurers provided similar data last year; overall, they had a small increase in election rate from 34.7 percent to 36.8 percent. By insurer, election rates varied from 13 percent to 91 percent. The insurers with the three lowest FPO election rates averaged a 25.8 percent election rate; they probably use a “positive election” approach. The other four insurers averaged 90.0 percent election; they probably use a “negative election” approach; i.e., the increase applies unless specifically rejected. The carrier which did not contribute such data last year caused the huge increase in election rate (Table 14); it probably uses a negative election rate.
Elimination Period
Table 15 summarizes the distribution of sales by facility elimination period. Ninety percent of buyers opt for 90-day elimination periods, however, two carriers report fewer than 60 percent of their policies have 90-day EPs (one has many shorter EPs and the other has many longer EPs). The percentage of purchasers buying 180-day or longer EPs hit a record (6.7 percent vs. 6.1 percent in 2012).
Table 16 shows that the percentage of policies with zero-day home care elimination period (but a longer facility elimination period), with adjustments for two carriers which reported only sales, but we know has either type of provision. With most insurers, fewer than 25 percent of buyers purchased a zero-day home care elimination period, but one insurer had nearly a 50 percent election rate.
The percentage of policies with a calendar-day elimination period (EP) definition (33.7 percent) also dropped back toward 2017 levels. For insurers which offer calendar-day EP, 79.4 percent of policies had the feature; in some cases, it was automatic. It is important to understand that most calendar-day EP provisions do not start counting until a paid-service day has occurred.
Sales to Couples and Gender Distribution
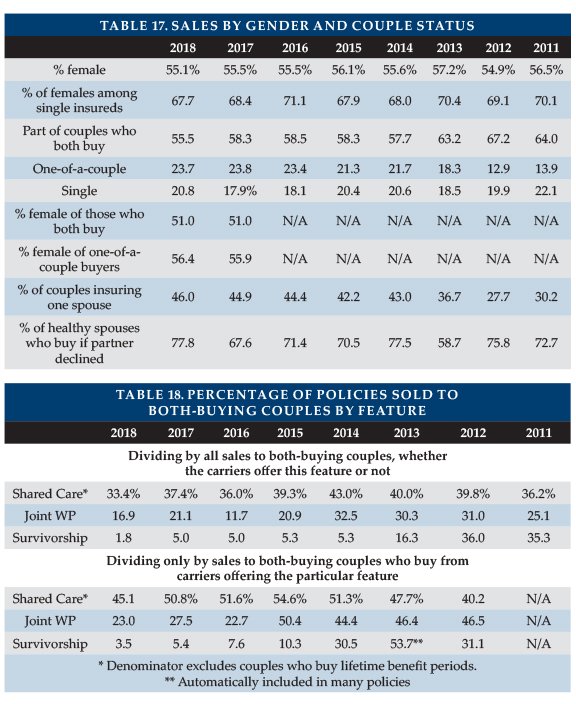
Table 17 summarizes the distribution of sales by gender and single/couple status.
The percentage of purchasers who consisted of couples who both buy (55.5 percent) and the percentage of all buyers who were female (67.7 percent) were the lowest percentages since at least 2010.
The 77.8 percent of accepted applicants who purchased coverage when their partners were declined was the highest over that time period. Three factors contributed approximately equally to the increase: General improvement; change of practice to allow a lower marital discount instead of no discount when one spouse is declined; and a change in participants reporting this data.
Fifty-five percent (55.1 percent) of all buyers were female, the lowest percentage since 2012. Insurers’ sales ranged from 47.2 percent female to 61.4 percent female, varying based on market (older age; fraternal, worksite vs. individual) and whether unisex rates were offered. Likewise, insurers ranged from 54.4 percent of single buyers being female to 79.8 percent.
Among couples, 51.0 percent are females, with insurers ranging from 47.9 percent (no other insurer showed less than 49.9 percent) to 52.1 percent. When only one of a couple buys, 56.4 percent are females, probably because the male partner is likely to be older and less likely to be insurable.
Shared Care and Other Couples’ Features
Table 18 summarizes sales of Shared Care and other couples’ features.
- Shared care—allows one spouse/partner to use the other’s available benefits if their own coverage has been depleted or offers a third independent pool that the couple can share.
- Survivorship—waives a survivor’s premium after the first death if specified conditions are met.
- Joint waiver of premium (WP)—both insureds’ premiums are waived if either qualifies for benefits.
Changes in distribution by carrier can greatly impact year-to-year comparisons in Table 18, because some insurers embed survivorship or joint waiver automatically (sometimes only in some circumstances) while others offer it for an extra premium or do not offer the feature. These percentages are lower than in the past, because one carrier reported the number of sales to couples last year, but not this year.
In the top half of Table 18, the percentages are based on the number of policies sold to couples who both buy. The bottom half of Table 18 shows the (higher) percentage that results from dividing the number of buyers by sales of insurers that offer the feature. Two insurers sold Joint WP to 56 to 60 percent of their couples and Survivorship to 10 to 12 percent of their couples.
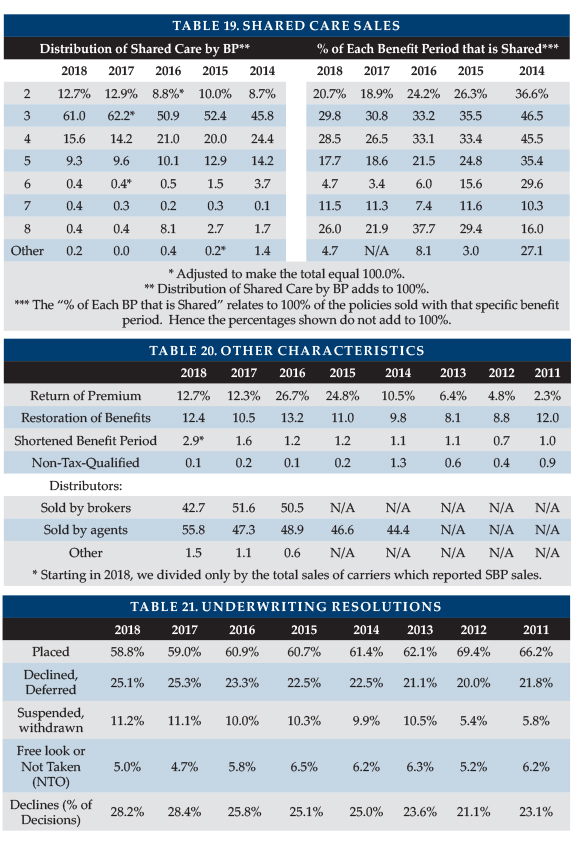
Table 19 provides additional breakdown on the characteristics of Shared Care sales. As shown on the right-hand side of Table 19, three-year and four-year benefit period policies are most likely (nearly 30 percent) to add Shared Care. Partly because three-year benefit periods comprise 50 percent of sales, most policies with Shared Care are three-year benefit period policies (61.1 percent, as shown on the left side of Table 20).
Above, we stated that Shared Care is selected by 33.4 percent of couples who both buy limited benefit period policies. However, Table 19 shows Shared Care comprised no more than 29.8 percent of any benefit period (it was elected by 25.4 percent of purchasers overall). Table 19 has lower percentages because Table 18 denominators are limited to people who buy with their spouse/partner whereas Table 19 denominators include all buyers. Shared care is more concentrated in two- to four-year benefits periods (89.4 percent of shared sales) than are all sales (72.6 percent). Couples seem more likely to buy short benefit periods, perhaps because couples plan to help provide care to each other, because Shared Care makes shorter benefit periods more acceptable and because single buyers are more likely to be female, hence opt for a longer benefit period. On the other hand, we also see a relatively high percentage of Shared Care on longer benefit periods; these people are probably trying to cover catastrophic risk and might prefer an endless benefit period. Some insurers were more likely to sell Shared Care on their short benefit-period policies, while others were more likely to sell Shared Care on their long benefit-period policies.
Existence and Type of Home Care Coverage
One participant reported home-care-only policies, which accounted for 0.7 percent of industry sales. Four participants reported sales of facility-only policies, which accounted for 0.9 percent of total sales. Ninety-five percent (95.1 percent) of the comprehensive policies included home care benefits at least equal to the facility benefit. These percentages are all lower than in 2017.
Partial cash alternative (and similar) features (which allow claimants, in lieu of any other benefit that month, to use between 30 percent and 40 percent of their benefits for whatever purpose they wish) were included in 41.3 percent of sales (lower than last year’s 44.1 percent).
Other Characteristics
As shown in Table 20, return of premium (ROP) features were included in 12.7 percent of all policies. ROP returns some or all premiums (usually reduced by paid LTCI benefits) when a policyholder dies. Approximately 79 percent of policies with ROP arise from ROP features embedded automatically in the product, compared to 93 percent in 2016. Embedded features are designed to raise premiums minimally, typically decreasing the ROP benefit to $0 by age 75.
Twelve percent (12.4 percent) of policies with limited benefit periods included a restoration of benefits (ROB) provision, which typically restores used benefits when the insured does not need services for at least six months. Approximately 87 percent of policies with ROB arose from ROB features automatically embedded, compared with 79 percent in 2016.
Shortened benefit period (SBP) nonforfeiture option was included in 1.8 percent of policies. Although every insurer is obligated to offer SBP, some carriers did not report any SBP sales. It seems appropriate to remove their sales from the denominator when determining the percentage of purchasers who selected SBP. On that basis, the percentage was 2.9 percent. Only one insurer reported a percentage above six percent (13.3 percent). SBP makes limited future LTCI benefits available to people who stop paying premiums after three or more years.
Only one insurer issued non-tax-qualified (NTQ) policies, which accounted for 0.1 percent of industry sales.
“Captive” (dedicated to one insurer) agents produced 55.8 percent of the policies. At one time, “captive” agents who sold LTCI tended to specialize in LTCI. Now many are agents of mutual companies. The 1.5 percent “other” sales did not involve a broker or agent.
Sales distribution by jurisdiction is posted on the Broker World website.
Limited Pay and Paid-Up Policies
In 2018, only two insurers sold policies that become paid-up, accounting for fewer than 0.5 percent of sales.
Because today’s prices are more stable, premium increases are less likely. One of the key reasons for buying 10-year-pay (avoidance of rate increases after the tenth year) is greatly reduced, while the cost of 10-year-pay has increased, making it less attractive than in the past. Nonetheless, limited-pay and single-pay policies are attractive to minimize post-retirement outflow and to accommodate §1035 exchanges.
Partnership Program Explanations
When someone applies to Medicaid for long term care services, states with Partnership programs disregard assets up to the amount of benefits received from a Partnership-qualified policy. Partnership sales were reported in 44 jurisdictions in 2018, all but Alaska, District of Columbia, Hawaii, Massachusetts, Mississippi, Utah, and Vermont, where Partnership programs do not exist. Massachusetts has a somewhat similar program (MassHealth).
The Partnership rules in California, Connecticut, Indiana and New York (“original” Partnership states) are significantly different than in other Partnership jurisdictions (“DRA” jurisdictions). The “original” states legislated variations of the Robert Woods Johnson Partnership proposal, whereas the “DRA” jurisdictions use more consistent rules based on the Deficit Reduction Act of 2005. For example, the “original” states require a separate Partnership policy form, generally still have more stringent benefit increase requirements and assess a fee for insurers to participate (none of which applies in DRA states). As a result, only two to four insurers sell Partnership policies in CA (2), CT (3), IN (4) and NY (2).
National Reciprocity Compact (NRC) requires member states to recognize Medicaid Asset Disregard earned in any other member state. States creating Partnerships under the Deficit Reduction Act of 2005 were automatically enrolled in the NRC but had the right to secede. The four original Partnership states (California, Connecticut, Indiana and New York) had the right to opt in. California is now the only jurisdiction with a Partnership program that is not a member of the NRC. However, New Hampshire (NH) created a unique regulation in 2018, limiting asset disregard related to policies sold in other jurisdictions to coverage issued on or after April 1, 2007, and only if the policy form was approved by the NH Insurance Department. We’ve asked NH about this regulation in 2018 and 2019, but have not received an explanation yet, so we’ll venture some thoughts below.
NH natives did not have an opportunity to purchase a Partnership policy until April 1, 2007. NH’s April 1, 2007, deviation from NRC standards seems intended to avoid extending asset disregard to an insured who moved in from another state if a NH resident who purchased on the same date can’t benefit from asset disregard.
The requirement that the policy form need have been approved by the NH Insurance Department is puzzling. Why should a NH citizen be harmed because they bought a policy as a resident of another jurisdiction? The impact may be limited because NH has been a member of the Interstate Insurance Product Regulation Commission since June 1, 2007. The IIPRC (“Compact”) approves LTCI policy forms for about 40 states. Policyholders with IIPRC-approved Partnership coverage issued since April 1, 2007, might still qualify for asset disregard if they move to NH.
It seems unlikely that individuals considering relocating to NH and their financial advisors will understand the potential Partnership ramifications. In the unlikely event that they are aware of NH’s unique law, it seems unlikely that they would know whether their policy form was approved by NH.
Partnership Program Sales
Insurers sometimes delay certifying policy forms as “Partnership” because of other priorities (e.g., needing time to comply with state-specific requirements to notify existing policyholders or offer an exchange). Such delay is not harmful, as certification is retroactive to policies already issued on that policy form if the policies have the required characteristics. For this reason and the “original” Partnership issues mentioned above, none of our participants sold Partnership policies in more than 40 jurisdictions in 2018. Five sold Partnership in 35-40 jurisdictions, three sold Partnership in 26-32 jurisdictions, one sold Partnership in eight jurisdictions, one in one jurisdiction (it sells in only one jurisdiction) and the other has never certified Partnership conformance and apparently does not intend to do so.
In the DRA states, 52.5 percent of policies qualified for Partnership status, whereas in the original states only 1.0 percent qualified. In Minnesota, more than 82 percent of the policies sold qualified as Partnership and Wisconsin and Wyoming both had 75 percent of their policies qualify.
Generally speaking, experts have expected Partnership policies to have higher average premiums because of the benefit increase requirements for Partnership policies. Only 26 of the 44 Partnership states demonstrated that pattern, with the other 18 having higher average premiums on non-Partnership policies.
In past survey articles, we noted that Partnership programs could be more successful if states broadened the eligibility requirements. Now, approximately 60 percent of Partnership states allow one percent compounding to qualify for Partnership, which can help low-budget buyers qualify for Partnership and also enables worksite core programs to be Partnership-qualified. A higher percentage of policies should qualify for Partnership in the future if insurers and advisors leverage these opportunities. Currently only three insurers offer one percent compounding.
Partnership programs could be more successful if:
- Advisors offer small maximum monthly benefits more frequently to the middle class. For example, a $1,500 initial maximum monthly benefit covers about four hours of home care every two days and, with compound benefit increases, may maintain buying power. Many middle-class citizens would like LTCI to help them stay at home while not “burning out” family caregivers and could be motivated further by Partnership asset disregard. (This approach does not work where a Partnership initial maximum monthly benefit must be at least $8608 (CT) and $9114 (NY). When policies reflecting CA SB 1248 become available in California, California’s minimum size policy will drop to $3000/month.)
- Middle-class clients were better educated about the importance of benefit increases to maintain LTCI purchasing power and to qualify for Partnership asset disregard.
- The four original Partnership steps migrate to DRA rules.
- More jurisdictions adopt Partnership programs.
- Programs that privately finance educational LTCI direct mail from public agencies were adopted more broadly.
- Financial advisors were to press reluctant insurers to certify their products.
- More financial advisors were certified. Some people argue that certification requirements should be loosened. At a minimum, the renewal certification process could be improved.
- More insurers offer one percent compounding.
- Combo products became Partnership-qualified.
Underwriting Data
Case Disposition
Ten insurers contributed application case disposition data to Table 21. In 2018, 58.8 percent of applications were placed, including those that were modified, a new low slightly below 2017’s previous record low of 59.0 percent.
One insurer reported a 77.1 percent placement rate; the second highest being 56.0 percent. The lowest placement rate was 34.0 percent. Low placement rates increase insurers’ cost per placed policy. More importantly, low placement rates can discourage advisors from discussing LTCI with clients. In addition to wasting time and effort encouraging clients to apply for LTCI, advisors fear disappointment for clients who are rejected.
Although the placement rate dipped slightly, the decline rate also dipped slightly to 25.1 percent of applications (28.2 percent of insurer decisions). Unfortunately, both the suspended/withdrawn and the Free Look refusals/not takens increased. The decline rate by carrier varied from 12.0 percent to 39.3 percent, affected by factors such as age distribution, market, underwriting requirements, underwriting standards.
Perhaps the best way to improve placement rates is to do a better job of pre-qualifying clients’ health profiles prior to submitting applications. General agencies and insurers are promoting approaches which make it easier for advisors to get detailed health information or have a third party ask health questions. For example, eApps should develop better health information and result in speedier processing which may help placement rates.
Our placed percentages reflect the insurers’ perspective. A higher percentage of applicants secure coverage because applicants denied by one carrier may be issued either stand-alone or combination coverage by another carrier or may receive coverage with the same insurer after a deferral period.
Underwriting Tools
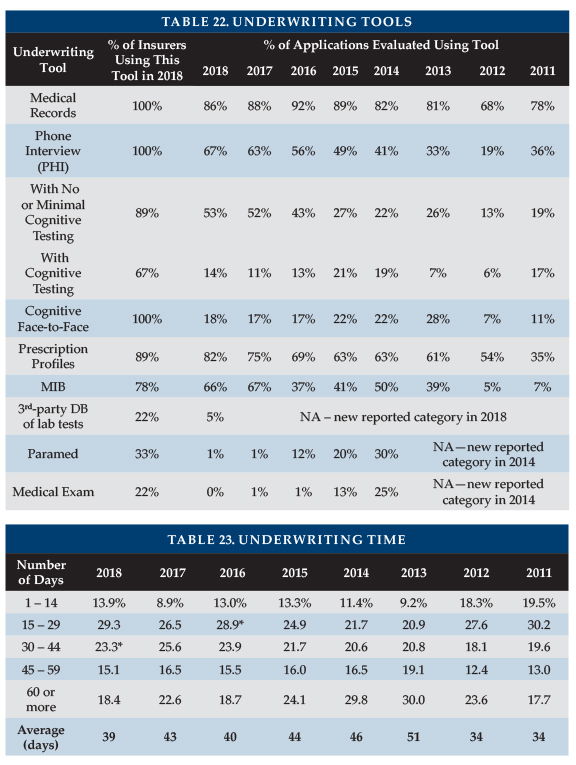
Nine insurers contributed data to Table 22, which divides the number of uses of each underwriting tool by the number of applications processed. For example, the number of medical records was 86 percent of the number of applications. That does not mean that 86 percent of the applications involved medical records, because some applications resulted in more than one set of medical records being requested.
Insurers are trying to speed underwriting to increase placement rates. Thus, phone interviews without cognitive screening, prescription profiles and MIB have increased significantly compared to levels of several years ago.
Year-to-year changes in distribution of sales among insurers significantly impact results. Lower maximum ages result in fewer face-to-face exams. Insurers might underreport the use of an underwriting tool because they may lack a good source for that statistic.
*MIB Underwriting Services alert underwriters to errors, omissions, misrepresentations and fraud on applications for life, health, disability income, long term care and critical illness coverage. MIB, Inc. provides its Underwriting Services exclusively to authorized individuals in MIB Group, Inc. member companies.
Underwriting Time
Table 23 shows that the average time from receipt of application to mailing the policy was the lowest since 2012. The improvement came at both ends of the spectrum, a much higher percentage processed within 29 days and many fewer taking 60 or more days. One insurer averaged only 29 days and four others average about 5 weeks or less. Three insurers averaged 51 to 59 days.
Rating Classification
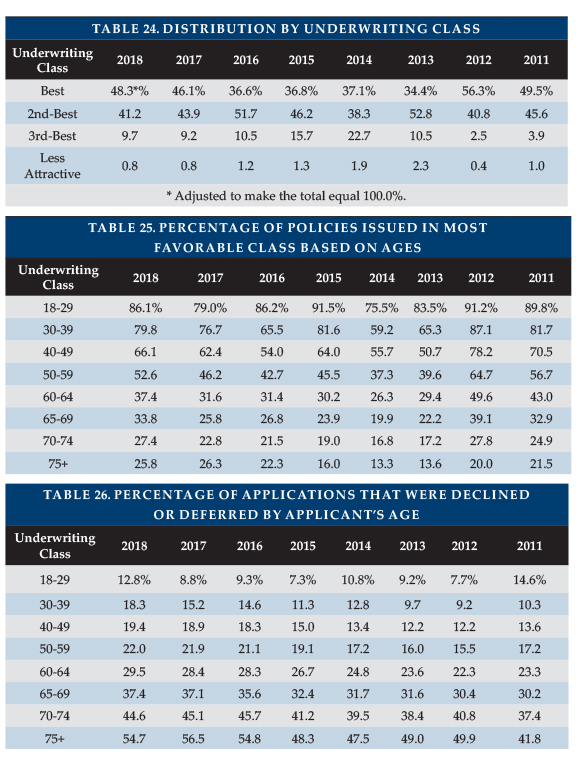
In 2017, a higher percentage of policies was issued in the most favorable rating classification (and in the top two most favorable rating classifications) than in any year since 2012. Table 24 shows 2018 showed similar results, with 48.3 percent in the most favorable classification and 89.5 percent of the policies in the two most favorable classifications. The “most-favorable” results in the past two years benefited from lack of reporting of rating classification distribution from insurers which do not offer preferred health discounts in the worksite and because one insurer eliminated its preferred health discount (hence “standard” ratings were its “best”). However, the reduction in the third-best and less attractive categories were not influenced by fewer worksite business participants being included in this part of the survey.
Table 25 shows that the percentage of policies issued in the most favorable category increased for each age range in 2018 and Table 26 shows that the decline rate went up in each age range except for ages 70+. Perhaps insurers are declining cases that previously might have been placed in the third-best or less attractive rating classifications. Tables 25 and 26 exclude most (perhaps all) policies underwritten with health concessions.
The by-age decline rates are a little high compared to the overall decline rate reported above. That’s because a significant carrier with a low decline rate was unable to provide their data by age.
Click here to view the following additional information available only online.
- Product Details, a row-by-row definition of the product exhibit entries, with a little commentary.
- Premium Exhibit, which shows lifetime annual premiums for each insurer’s most common underwriting class, for issue ages 40, 50, 60, and 70 for single females, single males, and heterosexual couples (assuming both buy at the same age), based on $100 per day (or closest equivalent monthly) benefit, 90-day facility and default home care elimination period (other aspects vary), three-year and five-year benefit periods or $100,000 and $200,000 maximum lifetime buckets, with and without Shared Care and with flat benefits or automatic three percent and five percent annual compound benefit increases for life. The exhibit includes facility-only policies, as well as comprehensive policies. Worksite products do not reflect any worksite-specific discount.
- Premium Adjustments (from our published prices) by underwriting class for each participant.
- Distribution by underwriting class for each participant.
- State-by-state results: percentage of sales by state, average premium by state and percentage of policies qualifying for Partnership by state.
Closing
We thank insurance company staff for submitting the data and responding to questions promptly. We also thank Nicole Gaspar and Alex Geanous of Milliman for managing the data expertly.
We reviewed data for reasonableness and insurers reviewed their product exhibit displays. Nonetheless, we cannot assure that all data is accurate.
If you have suggestions for improving this survey (including new entrants in the market), please contact one of the authors.
Footnote:
Society of Actuaries (November 2017). Long-Term Care Insurance: The SOA Pricing Project. Retrieved May 16, 2018, from https://www.soa.org/Files/Sections/ltc-pricing-project.pdf.






